How the four imperatives of precision, equity, ethics, and interoperability that we believe will define the technology foundation ACOs need to thrive in decade-long value-based programs.
What is intelligent health? It is how healthcare organizations use data, technology, and AI to deliver better care while managing costs effectively. According to Gartner report “Healthcare Provider Trends: Imperatives for Intelligent Health“, this approach provides a strategic roadmap for building the exact operational infrastructure that ACOs need to go beyond traditional operations and sustain performance over multiple years in long-term value-based contracts.
What Is Intelligent Health?
We believe intelligent health represents Gartner vision for AI-driven, hyper personalized healthcare delivery. It combines real-time decision making with continuous data insights and interoperable systems to create care experiences that are precise, equitable, ethical, and fully coordinated across all settings.
The insights rests on four imperatives that work together:
Precision: Exact, high-fidelity data that enables tailored treatments and optimized workflows
Equity: Eliminating unjust differences in healthcare access and outcomes
Ethics: Fair, transparent, and accountable use of AI and data
Interoperability: Seamless data exchange across all systems and organizations
These imperatives are not theoretical concepts. They directly address genuine operational challenges like clinician burnout, fragmented data, care gaps, and the shift to AI-augmented workflows that healthcare organizations are managing right now.

Why This Framework Matters for ACOs in Value-Based Programs?
ACOs operating under CMS quality payment programs face increasing accountability for total cost of care, health equity measures, and population health outcomes. Programs with multi-year commitments require infrastructure that can manage these demands consistently over time, not just for a single performance year.
The gap between what most ACOs have today and what they need is significant. Many organizations are still managing fragmented data across multiple systems, coordinating care through phone calls and faxes, and using retrospective analytics that identify problems only after they have already occurred.
In our view, the Gartner insights provide the building blocks to close that gap. Each imperative addresses specific operational requirements that CMS and other payers are actively measuring.
The Precision Imperative: Managing Total Cost of Care Proactively
Precision healthcare means having real-time, accurate data about your patient population and using it to make better decisions faster. For ACOs, this translates directly to prevent high-cost events before they happen.
A diabetic patient showing early signs of deterioration. With precision capabilities, you can identify that patient through predictive analytics, intervene with telehealth check-ins or care coordination, and prevent a hospitalization that would cost tens of thousands of dollars. Without precision capabilities, you only learn about the problem after the patient is already in the emergency department.
Gartner® identifies several foundational and transformational capabilities within the precision imperative:
• Real-time patient risk stratification across the full population
• Predictive analytics for high-cost event identification
• Command center intelligence for capacity management and resource optimization
• Precision medicine tools that tailor treatment to individual patient profiles and genetics
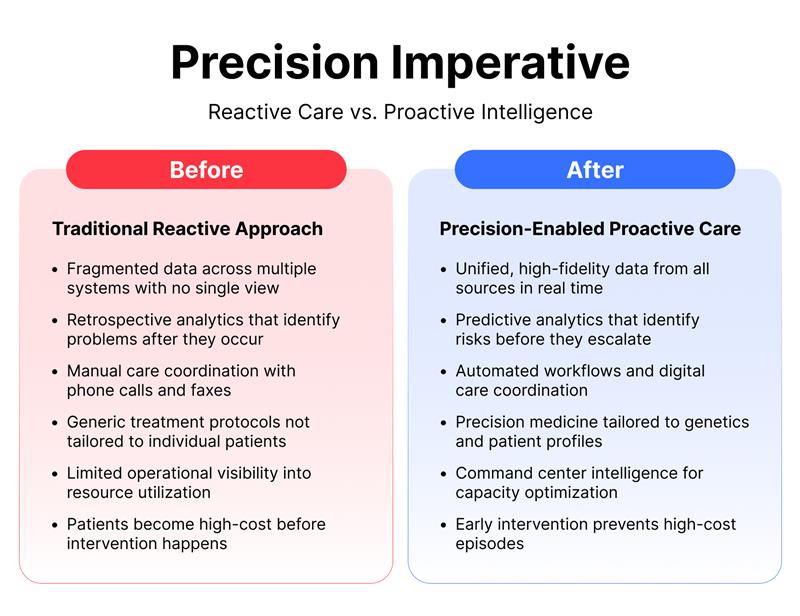
These capabilities are particularly critical for ACO care coordination strategies because they enable early intervention rather than reactive management.
The Equity Imperative: Meeting Mandatory Health Equity Requirements
Health equity means no unjust differences in healthcare access, inclusion, or outcomes. According to the World Health Organization, social determinants of health account for a significant portion of health disparities globally.
CMS has made health equity measurement mandatory in most value-based programs. ACOs must now collect social determinants of health data, monitor care gaps in underserved populations, and prove they are closing those gaps over time.
Most ACOs struggle here because SDoH data collection is inconsistent. Primary care clinics might be gathering this information, but specialists are not. Or the data is being collected but not used to drive actual interventions.
The equity imperative pushes organizations to fix these gaps through:
• Systematic SDoH monitoring across all patient touchpoints
• Health equity analytics that identify disparities by demographic group
• Targeted interventions for populations with the worst outcomes
• Digital literacy programs and multi-channel care access for diverse communities
Organizations that build these capabilities position themselves to succeed on CMS quality measures that increasingly emphasize equitable care delivery.
The Ethics Imperative: Building Trust in AI-Driven Care Delivery
Healthcare organizations are deploying AI tools at an accelerating pace. Predictive models, risk stratification algorithms, and automated care recommendations are becoming standard across the industry. But if care teams do not understand how these models work or do not trust the recommendations, adoption fails.
The ethics imperative is about deploying AI responsibly. That means:
• Explainable models where clinicians can see exactly why a patient was flagged
• Human-in-the-loop workflows so care decisions are not fully automated
• Bias testing across demographic groups to ensure equitable recommendations
• Transparency with patients about how their data is being used
ACOs will rely heavily on AI-powered tools to manage thousands of beneficiaries efficiently. But those capabilities need to be built in ways that clinicians trust and patients accept. Otherwise, technology becomes a barrier instead of an enabler.
The Interoperability Imperative: Enabling Seamless Care Coordination
Interoperability is the foundation that makes everything else possible. Long-term value-based contracts require ACOs to manage care across the entire continuum: primary care, specialists, hospitals, post-acute, home health, and beyond. That only works if data flows seamlessly across all those settings.
Right now, most ACOs are dealing with faxed referrals, phone calls to track down test results, and fragmented views of what is happening with patients outside their own network. These manual processes waste time, increase errors, and prevent the kind of coordinated care that value-based programs require.
We feel the Gartner interoperability imperative pushes organizations to adopt modern standards:
• FHIR-based data exchange that replaces fax and phone-based workflows
• Active participation in health information exchanges
• Real-time ADT notifications when patients are admitted or discharged
• API-first vendor requirements for all new technology purchases
When interoperability works, care managers get automatic alerts when a patient is hospitalized, lab results flow into the system without manual entry, and the entire care team has a complete picture of each patient’s journey. That level of visibility is essential for effective population health management.

Getting Started with Intelligent Health Infrastructure
Organizations preparing for long-term value-based contracts should assess their current capabilities against each imperative. Start by identifying the biggest gaps that directly impact performance metrics. Then prioritize investments in platforms that address multiple imperatives simultaneously rather than deploying separate point solutions for each problem.
The infrastructure decisions you make now will determine whether your organization can sustain performance over multi-year contracts or will spend years playing catch-up while competitors pull ahead.
Frequently Asked Questions
What is intelligent health in healthcare?
Gartner provides insights for AI-driven, hyper personalized healthcare delivery that combines real-time decision making with continuous data insights. It is built on four imperatives: precision, equity, ethics, and interoperability working together to create coordinated, effective care.
Why is interoperability important for ACOs?
Interoperability enables seamless data exchange across all care settings, which is essential for coordinating care in value-based programs. Without interoperability, ACOs cannot effectively manage patients across hospitals, specialists, post-acute facilities, and primary care, leading to care gaps and preventable costs.
What are social determinants of health (SDoH)?
Social determinants of health are non-medical factors that influence health outcomes, including economic stability, education access, social and community context, healthcare access, and neighborhood environment. CMS requires ACOs to collect and act on SDoH data to address health equity.
How does AI support value-based care delivery?
AI enables predictive analytics for identifying high-risk patients before costly events occur, automates care gap identification, optimizes resource allocation, and provides real-time operational intelligence. When deployed ethically with explainable models and human oversight, AI helps ACOs manage large populations efficiently.
What is FHIR and why does it matter for healthcare?
Fast Healthcare Interoperability Resources (FHIR) is a modern data exchange standard that enables real-time data sharing across healthcare systems. FHIR replaces outdated fax and phone-based workflows with API-based integration, making care coordination significantly more efficient for ACOs and health systems.
What infrastructure do ACOs need for long-term value-based contracts?
ACOs need unified platforms that provide real-time risk stratification, SDoH monitoring, predictive analytics, care coordination tools, health equity reporting, and interoperable data exchange. These capabilities must work together rather than existing as separate point solutions to effectively manage decade-long value-based commitments.
How can ACOs assess their intelligent health readiness?
ACOs should evaluate their current capabilities across all four imperatives: precision (real-time analytics and risk stratification), equity (SDoH data collection and disparity monitoring), ethics (explainable AI and governance frameworks), and interoperability (FHIR adoption and HIE participation). Organizations scoring low across these areas should prioritize infrastructure modernization.
How to assess your organization’s intelligent health readiness? Contact our team to learn how CareSpace® enables all four imperatives in a single platform designed for value-based care success.
Table of Contents
